On September 8, 2015, during a session in the European Congress on Tropical Medicine and International Health, Médecins Sans Frontières (Doctors Without Borders) sounded a warning that stockpiles of the antivenom which is most effective against several of Africa’s poisonous snakes would run out. Médecins Sans Frontières estimated this would cause an additional 10,000 deaths in Africa each year.
 It’s unclear how many were dying already. Médecins Sans Frontières estimates that there are about 30,000 deaths and 8,000 amputations as a result of snakebites in Sub-Saharan Africa each year. The World Health Organization reports about 5 million snakebites each year result in over 100,00 deaths worldwide. Treatment is important: 10-15% of people with an untreated snakebite will die. With antivenom drugs, only 0.5% die. As David Williams, a toxicologist & herpetologist at University of Melbourne & chief executive of non-profit organization Global Snakebite Initiative, says of untreated snakebites: “It’s the most neglected of the world’s most neglected tropical diseases.”
It’s unclear how many were dying already. Médecins Sans Frontières estimates that there are about 30,000 deaths and 8,000 amputations as a result of snakebites in Sub-Saharan Africa each year. The World Health Organization reports about 5 million snakebites each year result in over 100,00 deaths worldwide. Treatment is important: 10-15% of people with an untreated snakebite will die. With antivenom drugs, only 0.5% die. As David Williams, a toxicologist & herpetologist at University of Melbourne & chief executive of non-profit organization Global Snakebite Initiative, says of untreated snakebites: “It’s the most neglected of the world’s most neglected tropical diseases.”
This situation results in a significant impact to safety. The deaths and amputations result from inadequately treated snakebite. There are two parts to the cause-and-effect: the snakebite, and the treatment. Snakebite results when a person is bitten by a venomous snake because that person and the snake are in the same vicinity (typically a field where the person is farming) and some part of the person’s skin is exposed. A common cause is a farmer who is not wearing boots because they are unaffordable.
Inadequate treatment of snakebite victims can result from antivenom not being readily available, but also can result from ineffective clinical application. Lack of training of healthcare personnel (the World Health Organization has no formal training program for snakebite. (It does for 17 other neglected tropical diseases, but snakebite causes more deaths than all 17 of these put together, according to tropical-medicine specialist David Warrell of the University of Oxford.) The proliferation of counterfeit antivenom has also likely caused many to doubt the efficacy of antivenom.
However, the primary issue is when antivenom isn’t available at all. Even before the warning, only about 10% of Africa’s snakebite victims received antivenom. The alarm was sounded because the company that makes the most effective antivenom (which can treat bites from many of Africa’s venomous snakes) stopped production in 2010. The company said cheaper products by competitors have forced it out of the market, though it’s working to transfer production capability to another company. A big concern facing producers is the unreliable market – hospitals and clinics don’t always have antivenom.
Concerns facing hospitals and clinics are that most products (unlike the one taken off the market in 2010) work against only one species of snake, so multiple antivenom products have to be kept on hand. These products have a limited shelf life and require continuous refrigeration. While the drugs themselves are inexpensive, corruption and bribery can increase the cost to hospitals and clinics significantly. Some patients can’t pay for it, and some won’t, likely because they doubt its efficacy, thanks to counterfeits that have surged due to inadequate oversight. (Although there are venomous snakes, there’s less of an issue in Latin America because most governments produce and distribute antivenom. Various Latin American governments are working to help Africa with snakebite treatments.)
What else is needed? Well, with a problem this complex, multiple solutions to address different causes will be required. Health experts and the Global Snakebite Initiative are working towards the creation of a universal antivenom, with hopes that governments will step in to aid in the development, production and distribution of antivenom drugs. Public outreach and training for health care personnel as to the safety and efficacy of antivenom are also needed. Those on the front lines say that even providing boots would help. Says Abdulsalam Nasidi, who worked for Nigeria’s Federal Ministry of Health, “It’s perhaps the ultimate in low-tech methods in snakebite protection: shielding vulnerable human skin.”
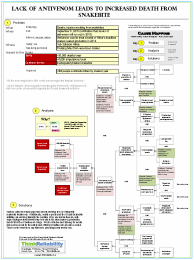
View a Cause Map, a visual root cause analysis made up of cause-and-effect relationships, for this issue by clicking on the thumbnail above. Or, click here to learn more about this issue and the Global Snakebite Initiative.











