 Having surgery is always a little scary and never fun, but imagine waking up after the procedure to learn that you never needed the operation in the first place. This is exactly what happened to a patient in Worcester, Massachusetts. The patient had surgery to remove a kidney that was believed to have a large tumor. After the procedure, the removed kidney was found to be healthy without any tumors. Investigators found that the surgery had been performed on the wrong patient.
Having surgery is always a little scary and never fun, but imagine waking up after the procedure to learn that you never needed the operation in the first place. This is exactly what happened to a patient in Worcester, Massachusetts. The patient had surgery to remove a kidney that was believed to have a large tumor. After the procedure, the removed kidney was found to be healthy without any tumors. Investigators found that the surgery had been performed on the wrong patient.
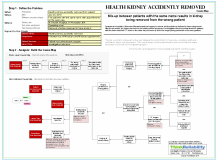
So what went wrong? Cause Mapping, a visual format for performing a root cause analysis, can be used to help illustrate this issue. In Cause Mapping, all the causes that contributed to an issue are visually laid out to intuitively show the cause-and-effect relationships. The first step in Cause Mapping is to define the problem by filling in an Outline with the basic background information, such as the date, time and location. In addition, the Outline is used to document how the problem impacted the overall goals. For example, in this case the patient services goal is impacted because a patient had unnecessary surgery and the compliance goal is impacted because the hospital faces potential loss of Medicare and Medicaid agreements as a result of this medical error if they do not implement corrective actions in a timely manner. Most issues impact more than one goal of an organization and identifying the areas of concern at the start of the investigation helps ensure that all facets of the issue are considered during the investigation.
Once the Outline is filled out, the Cause Map itself is built by starting at one impacted goal and asking “Why?” questions. So why did a patient have unnecessary surgery? Doctors had identified a large tumor in a patient’s kidney and decided the best course of treatment was to remove the kidney, but the surgery was performed on the wrong patient. Details about exactly how the initial patient misidentification occurred have not been released, but it is known that two patients with the same name both had CT scans at the same facility on the same day. The CT scans were not performed at the hospital that performed the surgery.
The identification checks done at the hospital that performed the surgery were inadequate to catch the error prior to the surgery being performed. Only the patient name was used to confirm identify. Proper patient identification procedure requires a second identifier, such as birthdate, be used to confirm patient identify. There is some conflicting information in media articles on this incident, but it also appears that the patient’s file did not contain the CT scan and that surgical staff failed to confirm the CT image prior to performing the survey.
It’s easy to see how patients with the same name could increase the likelihood of a mix-up, but there were several places in the work flow where the patient’s identity should have been confirmed and the error caught before the healthy kidney was removed. None of them caught the error. The hospital is working to improve reliability in their processes to prevent a similar error from occurring in the future. The computers in the surgery room have been changed so that they show the patient’s name AND birthdate instead of only the patient’s name to help ensure a second patient identifier is used to confirm identity prior to performing surgeries. The hospital also plans to increase staff training on how to correctly identify patients and the need to ensure that all test results are on hand before a surgery can proceed.